Source: The Guardian.
Maternal health in the Democratic Republic of the Congo is undermined by a lack of awareness and access to healthcare.
Her eyes wide with fear and pain, Théthé – who is haemorrhaging and has a fever – groans and pushes as she lies on a brown vinyl mattress, slick with blood and amniotic fluid, in one of the worst places in the world to be a mother (pdf). After a final push, a nurse holds up a waxy baby girl by the feet. Her arms hang limp, her skin an opaque bluish-pink. « Stillborn, » says Kavita Masenga, the lead obstetric nurse.
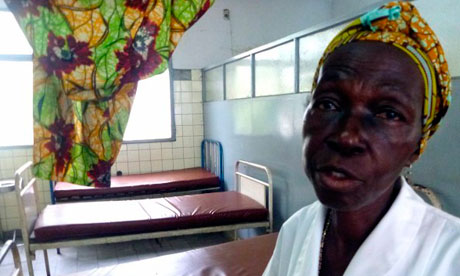
Such outcomes are routine at Kinshasa general hospital, the main referral hospital in the capital of the Democratic Republic of the Congo (DRC). The most serious obstetric cases in this traffic-clogged city of 10 million people are sent here.
Although conditions have improved in recent years, the hospital remains plagued by the country’s problems: power cuts, outdated equipment, poorly-paid staff and drug shortages. Years of corrupt leadership and low levels of investment in health have taken a toll.
Over her lifetime, a Congolese woman faces a one in 24 chance of dying from complications arising from pregnancy or childbirth. In several interviews with medical workers in Kinshasa, they all cited poverty as the main trigger of maternal deaths. Three-quarters of Congolese women who did not give birth in a health facility cited lack of funds to pay for services as the reason, according to a World Bank survey.
« In some places, when you arrive [for care] and you don’t have money, they just transfer you and transfer you. That is part of the reason we have such a high rate of maternal mortality in our country, » said Dr Blandine Aveledi, reproductive health manager for the New York-based International Rescue Committee (IRC) in Kinshasa. « The greatest problem is access to finances. »
Hard-pressed Congolese health professionals say the country should do better. It possesses vast quantities of diamonds, gold, copper, timber, rubber and other resources. But it ranks at the bottom of UN indicators for human development. According to the World Bank, Congo is one of only nine countries where life expectancy has fallen below 1970 levels.
« You cannot tell me my government is so poor, when I see [government] ministers and the number of cars they have, the numbers of villas. When I see that – you want to tell me that they don’t have money for the health problems in the country? » said an indignant Dr Mbwebwe Kabamba, head of the emergency department at Kinshasa general.
Health experts say that closely spaced pregnancies are one of the largest factors in both maternal and child deaths, regardless of whether a woman has access to healthcare. But only 6% of women use modern methods of contraception, according to Save the Children. For birth control, cost is not the major barrier. An intrauterine device, for example, costs between $1 and $2.50, and a contraceptive injection between 50 cents and $1.50. A larger problem is awareness and access, says Dr Leon Kintaudi of Sanru, a Kinshasa-based rural health programme.
The secretary general in the ministry of public health, Dr Pierre Lokadi Otete Opetha, said about 5% of the country’s budget last year was set aside for healthcare. This compares with between 15% and 20% for developed countries, and is well below the minimum figure agreed by the 2001 Abuja declaration, which committed African governments to allocate 15% of their national budgets to health.
But Opetha insisted his government is committed to improving maternal health in the DRC. He said expanding family planning services, which would save the lives of both mothers and babies, is a major focus.
« It’s a priority of the head of state [President Joseph Kabila], » he said. « I remember at many meetings that he comes back to that. As there is the high-level political will, and with our partners, I think from this year there will be a kicking off of family planning efforts. »
The average Congolese woman bears six children. For women who survive pregnancy and childbirth, each new baby increases her family’s struggle to feed and educate them.
At the Roi Baudouin hospital in a crowded suburb of Kinshasa, 33-year-old Olivie Kasongo has had her second set of twins. Now she has seven children, and the family lives on a policeman’s salary of about $30 a month.
« It is very difficult because the children – you must educate them, feed them, » she says. « I’ll come back to [the hospital] to do the family planning. I’m going to speak to my husband and he must accept it. »
The reality, doctors say, is he probably won’t. But until family planning becomes more widely available and more widely used in Congo, dangerous illegal abortions are likely to remain the leading method of birth control, according to health workers. Until then, they expect that Kinshasa general will continue to see a steady stream of mothers like Théthé.




